In 1997 it was published a paper concerning the use of intravenously (IV) cefuroxime prophylaxis against nosocomial pneumonia in intubated patients with structural coma.1 This randomized clinical trial (RCT) studied two groups of patients: one of them were administered two doses of IV cefuroxime upon intubation, and the other were administered no antibiotic prophylaxis. A 52% reduction was observed in ventilator-associated pneumonia (VAP) and 56% if early-onset ventilator-associated pneumonia (EO-VAP) is considered in the IV cefuroxime prophylaxis group. Since then, several research groups worldwide have followed this clinical practice on intubated patients with structural coma upon intubation. Now, literature is reviewed to check whether this measure is still appropriate twenty years later, and some criticism is also made regarding the inclusion of this preventive measure into international recommendations and guidelines for infection control of intubated patients in intensive care units (ICU).2
The main findings of the pilot studyComa patients – mainly from traumatic brain injury, when tracheal intubation has been performed – have a high risk for developing VAP and specially EO-VAP in the first five days, and microorganisms that could be called “community”, such as methicillin-sensitive Staphylococcus aureus, Haemophilus influenzae and Streptococcus pneumoniae, which are already colonizing the upper airways at the time of intubation. The initial hypothesis in the pilot study1 was that prophylactic cefuroxime in two IV doses during the first 24h could be an effective preventive measure against VAP.
A RCT was designed to reduce VAP incidence in intubated patients with head injury or medical stroke requiring over 48h of mechanical ventilation. One hundred patients were included (they had head injury or coma caused by stroke) and with Glasgow coma scores (GCS) ≤12 points. Patients eligible for the study (no=50) were given two 1.5g doses of IV cefuroxime every 12h upon intubation (cefuroxime group), and 50 patients, who were given no cefuroxime, formed the control group. VAP diagnosis was completed by protected bronchoalveolar mini-lavage with microscopic examination of intracellular organisms and quantitative culture.3 The global incidence of microbiologically confirmed VAP was 37% (n=37); 12 (24%) patients belonged to the cefuroxime group, and 25 (50%) patients belonged to the control group (p=0.007). EO-VAP accounted for 70% of all VAP episodes (n=26), eight belonging to the cefuroxime group, and 18 belonging to the control group (p=0.02). Multivariate analysis revealed that the use of cefuroxime had a protective effect against VAP development. No differences were found with regard to mortality and morbidity when the study population was compared with the control group. The administration of two single high doses of 1.5g each of IV cefuroxime after the intubation of patients with structural coma due to head injury or medical stroke was proven an effective prophylactic strategy to reduce VAP incidence This prevention was also observed to improve EO-VAP incidence.
Publications on this topic since the initial studyThe reality is that the pilot study has been cited many times over the later years, but only two investigations tested a similar hypothesis, but with different protocols. In this line, Acquarolo et al.4 aimed to evaluate whether a 3-day ampicillin-sulbactam prophylaxis could reduce EO-VAP occurrence in comatose (GCS≤8) mechanically-ventilated patients. This was a single centre, prospective, randomized, open study in a general neurological ICU. Patients were randomized to either IV ampicillin-sulbactam prophylaxis (3g every 6h for 3 days) plus standard treatment or standard treatment alone. The 1-year interim analysis showed that ampicillin-sulbactam significantly reduced EO-VAP occurrence, and the study was stopped after 42 patients had been enrolled. A total of 38 patients were included in the final analysis; 15 out of these 38 patients (39.5%) developed EO-VAP: 11 (57.9%) in the standard treatment group and 4 (21.0%) in the ampicillin-sulbactam group (p=0.022). In conclusion, this prospective, randomized, open study found out that 3-day ampicillin-sulbactam prophylaxis in critically-ill mechanically-ventilated comatose patients reduces EO-VAP occurrence by 64%. This study was published seven years later and is one whose hpothesis is most similar to the initial hypothesis, but it uses a broad-spectrum antibiotic, and for longer days. The number of patients included was less than half of those in the initial pilot study.
A second study was published sixteen years later by Vallés et al.5 It was a comparative study of two historical cohorts: a non-prophylaxis (58 patients) group and a prophylaxis group (71 patients): a single 2g dose of IV ceftriaxone. The incidence of microbiologically probed EO-VAP was 2 out of 71 (2.8%) in the prophylaxis group compared with 13 out of 58 (22.4%) in the control group (p=0.001). These results proved the effectiveness of a single dose of antibiotic for prophylaxis against EO-VAP in this concrete group of comatose patients.
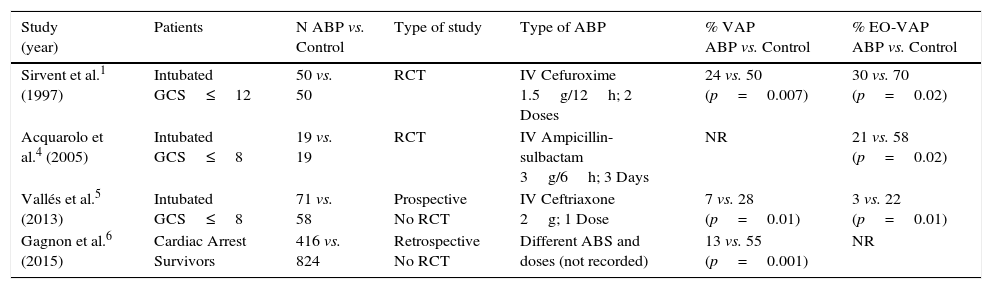
Another study with a similar hypothesis performed in survivors of cardiac arrest is the work of Gagnon et al.6 The Northern Hypothermia Network registry data was used to complete a retrospective cohort study comparing patients treated with antibiotic prophylaxis (different antibiotics and doses) with patients receiving no antibiotic prophylaxis. They included cardiac arrest survivors with a GCS ≤8 upon hospital admission treated with hypothermia at 32–34°C. They studied 1240 patients. The prophylaxis group showed lower incidence of pneumonia (12.6% vs. 54.9%, p<0.001) compared to no-prophylaxis patients. In addition, logistic regression proved that antibiotic prophylaxis was independently-associated to a lower incidence of pneumonia (OR: 0.09; 95%CI: 0.06–0.14; p<0.001), and a similar incidence of good functional outcome. The limitations of this study is that – as a retrospective cohort study – it examined data from a multinational, web-based registry of post-resuscitation cardiac arrest care to study different types of antibiotic and doses, this essential topic not being included in the study. A summary of the features of these studies is shown in Table 1.
Characteristics of the studies on antibiotic prophylaxis against VAP in coma patients.
| Study (year) | Patients | N ABP vs. Control | Type of study | Type of ABP | % VAP ABP vs. Control | % EO-VAP ABP vs. Control |
|---|---|---|---|---|---|---|
| Sirvent et al.1 (1997) | Intubated GCS≤12 | 50 vs. 50 | RCT | IV Cefuroxime 1.5g/12h; 2 Doses | 24 vs. 50 (p=0.007) | 30 vs. 70 (p=0.02) |
| Acquarolo et al.4 (2005) | Intubated GCS≤8 | 19 vs. 19 | RCT | IV Ampicillin-sulbactam 3g/6h; 3 Days | NR | 21 vs. 58 (p=0.02) |
| Vallés et al.5 (2013) | Intubated GCS≤8 | 71 vs. 58 | Prospective No RCT | IV Ceftriaxone 2g; 1 Dose | 7 vs. 28 (p=0.01) | 3 vs. 22 (p=0.01) |
| Gagnon et al.6 (2015) | Cardiac Arrest Survivors | 416 vs. 824 | Retrospective No RCT | Different ABS and doses (not recorded) | 13 vs. 55 (p=0.001) | NR |
RCT: Randomized Clinical Trial; GCS: Glasgow Coma Score; IV: intravenously; ABP: antibiotic prophylaxis; ABS: antibiotics; VAP: ventilator-associated pneumonia; EO-VAP: early-onset ventilator-associated pneumonia; NR: not reported.
Over the years, since the publication of the initial RCT, there have been various international initiatives to implement this preventive strategy against VAP. Different guidelines recommend several strategies for VAP prevention. The guidelines of the American Thoracic Society/Infectious Diseases Society of America (ATS/IDSA)7 conclude, from level-1 evidence based on a single, prospective, randomized, clinical trial,1 that the prophylactic administration of a systemic antibiotic for 24h at the time of emergent intubation may be useful to prevent VAP in patients with closed head injury. However, these American guidelines have not yet recommended the prophylactic use of systemic antibiotics for all intubated patients, which awaits the availability of further data. However, recent ATS/IDSA 2016 guidelines8 only discuss recommendations on VAP diagnosis and antibiotic treatment. These current guidelines mention no prevention measures for nosocomial pneumonia.
In 2007, the Brain Trauma Foundation published the 3rd edition of its Guidelines for the management of severe traumatic brain injury,9 describing the results of this initial RCT, and suggests the immediate application of this pharmacological measure to reduce VAP incidence in intubated traumatic brain injury patients.
From a European perspective, guidelines published in 200910 present the short course of IV antibiotics as a strategy that requires further study to be systematically recommended in intubated patients for VAP prevention.
A very interesting initiative to reduce VAP has recently been developed by the Spanish Societies of Intensive Care Medicine and Intensive Care Nursing, being defined as “Zero-VAP”,2 which proposed the implementation of a simultaneous multimodal intervention in ICU consisting of a bundle of VAP prevention measures. The “Zero-VAP” Project incorporates an integral patient safety programme and continuous online validation of bundle application. The implementation of the guidelines aims at reducing VAP to less than 9 episodes per 1000 days of mechanical ventilation. A total of 35 preventive measures were initially selected. A group of experts have generated a list of 7 basic mandatory recommendations: education and training in airway management, strict hand hygiene for airway management, cuff pressure control, oral hygiene with chlorhexidine, semi-recumbent positioning, promotion of measures to safely avoid or reduce time on ventilator, and discouragement of scheduled changes of ventilator circuits, humidifiers and endotracheal tubes; as well as 3 additional highly-recommended measures: selective digestive-tract decontamination, aspiration of subglottic secretions, and a short course of IV antibiotic.
After a review of literature and the international guidelines that have been published since the publication of the initial work, the question that we make is: where are we now? The answer is simple. Since the single RCT study performed twenty years ago, the current clinical practice has changed and there is no uniform management of intubated patients with coma. The fact that the type and dose of IV antibiotic was different in all the aforementioned studies suggests that the positive effect of IV antibiotic prophylaxis depends more on immediate administration upon intubation – to counteract bacterial inoculum in the upper airways – than on antibiotic type and dose. This preventive measure may now be obsolete due to changes in the colonizing microorganisms of the population or due to a multifactorial behaviour in VAP development in coma patients. It is surprising that, throughout all these years, no research has been focused on this hypothesis and tested this or any other antibiotic using a large randomized clinical trial.
New strategies for future research in antibiotic prophylaxis against VAPPatients with structural coma, usually due to traumatic head injury, are nearly always intubated in emergency conditions outside the hospital, where the lack of aseptic conditions makes it easier for microorganisms to enter the respiratory tract. In the initial study, trachea colonization within 24h of intubation by “community microorganisms” was observed to be a risk factor for EO-VAP development in patients with head trauma. Due to this fact, in the last years an increase in the etiologic cause of EO-VAP has been observed due to enteric bacteria from gastrointestinal microbiota, commonly resistant to cefuroxime or/and amoxicillin-clavulanic acid. Furthermore, high oxygen tension in ventilated patients is enough to kill anaerobes and – in this situation of new microbiology patterns of VAP – we and others propose the use of other antibiotics rather than cefuroxime for prophylaxis and for treatment of aspiration pneumonia,11 which is the pathogenic basis of EO-VAP in intubated patients with altered level of consciousness.
Consequently, we believe that it is time to risk a change to an antibiotic prophylaxis which is likely to be more effective against aerobic gram-positive and enteric gram-negative bacilli, as well as a change in terms of pharmacokinetics and pharmacodynamics with a more adequate spectrum to the current aetiology of EO-VAP in recently-intubated coma patients. However, the effect of this prophylactic measure on the development of bacterial resistance must always be monitored periodically to detect prophilaxis-related bacterial resistance if its use is not appropriate. Thus, antibiotic prophylaxis for >48h has been shown a practice significantly associated with clinical complications related to nosocomial pneumonia.12
ConclusionAfter 20 years of the IV antibiotic prophylaxis for VAP prevention in intubated coma patients, perhaps it is time to launch a large RCT to evaluate other types of antibiotic prophylaxis with no effect on normal anaerobic microbiota and with a broad-spectrum to Gram-positive and enteric Gram-negative bacilli. However, attention must be paid to the evolution of resistant micro-organisms, and maintaining this antibiotic prophylaxis for more days than planned should be avoided.
Conflict of interestThe authors declare no conflict of interest.
The author thanks the team of physicians and nurses in our ICU for their professional care of critically-ill patients and their families. I also thank Dr. J.M. Fernández-Real for his help revising the manuscript.