The risk of thrombotic events increases in patients with SARS-CoV-2 (COVID-1)-induced pneumonia.1,2 Clinical practice guidelines and scientific societies simply do not agree on their recommendations for the management and prevention of these events. Therefore, the Spanish Society of Intensive and Critical Care Medicine and Coronary Units (SEMICYUC) has proposed adjusting the dosage of low molecular weight heparin (LMWH) by obtaining the Anti-Xa factor levels.3,4 While they justified this recommendation due to the high risk of thrombotic/hemorrhagic events and the rate of under/overdose (23% and 46%), the level of evidence granted was C-III (weak support for the recommendation based on expert opinions or descriptive studies). The utility of this strategy to reduce these complications, and to determine the appropriate levels, is controversial.3,5–7 The objectives of our study were to assess the adjustment of prophylactic enoxaparin by Anti-Xa factor, the levels obtained, and the presence of possible risk factors associated with overdose in patients admitted to the ICU with COVID-19-induced pneumonia.
We conducted an observational and retrospective study at the ICU of a tertiary care level hospital from July 2020 through February 2021. Consecutive critically ill patients with COVID-19-induced pneumonia were evaluated in whom the prophylactic enoxaparin dose was directed by the Anti-Xa factor levels. The inclusion criteria were: (1) patients with COVID-19-induced pneumonia (presence of radiological infiltrates and positive PCR test for SARS-CoV-2 in respiratory samples); (2) need for respiratory support (high-flow oxygen therapy, non-invasive support, or invasive mechanical ventilation); (3) adjustment of prophylactic enoxaparin dosage directed by Anti-Xa factor. Cases with an initial therapeutic indication were excluded. In those patients who modified their regimen from prophylactic to therapeutic during admission, the doses and levels were both included, as well as thrombotic/hemorrhagic complications during the prophylaxis period.
The protocol of our center for initial enoxaparin doses consisted of (1) standard dose of 40mg/24h; (2) dose of 60mg/24h in patients with body mass index (BMI) > 30 or elevated acute phase reactants (D-dimer levels >1500ng/mL and C-reactive protein >150mg/L); (3) dose of 80mg/24h if both risk factors were present (BMI+elevated reactants). In case of kidney disease, dosage was reduced based on creatinine clearance. Afterwards, the dose was adjusted based on the Anti-Xa levels. In addition, given the high risk of thrombosis reported, target range from 0.30 IU/mL to 0.59 IU/mL were agreed upon by a multidisciplinary team, which are similar target range compared to those from former studies.1,6,7 Measurements were taken in a sort of treatment balance state of enoxaparin (48h–72h without dose changes) and in a peak phase, 3h–5h after the administration. They were periodically repeated every 2–3 days depending on the patients’ clinical situation and response to treatment.
Variables associated with demographics, comorbidities, severity at the ICU admission, lab test results, treatment, and need for support were all collected. The outcomes "thrombotic events" at the ICU stay (deep vein thrombosis and/or acute pulmonary thromboembolism diagnosed through imaging modalities requested at the doctor’s discretion), "hemorrhagic events" (severe: critical location, reduction of Hb by 2g/dL or transfusion of 2 units of red blood cells), and mortality at the ICU stay were also recorded. Regarding the statistical analysis, the categorical variables were expressed as absolute value and percentage and compared using the chi-square test or Fisher's exact test. The continuous ones were expressed as median while 25th-75th percentiles were compared using the Student t test, or the Mann-Whitney U test when the variables did not have a normal distribution. The factors associated with dependent variables "Anti-Xa levels ≥0.60 IU/mL" (values above the target range) and "thrombotic events" were analyzed through multivariable logistic regression studies. Variables with P values <.2 or of greater clinical interest were explored. The cut-off value for continuous variables was adjusted using the Youden index method.
A total of 160 critically ill patients with COVID-19-induced pneumonia on enoxaparin prophylaxis were included in the study, and a total of 589 Anti-Xa factor determinations were performed. The patients’ median age was 63 years being obesity the most common comorbidity of all (67%, [n=107/160]), and showing rates of creatinine clearance <30mL/min at admission of 6% (10/160). The median of D-dimer values at admission were 1242ng/mL (p25−75, 704−3765) with 58% (94/160) requiring invasive mechanical ventilation. The mortality rate at the ICU stay was 28% (45/160) with rates of diagnosed thrombotic events and severe bleeding of 9% (15/160) and 4% (7/160), respectively (Table 1).
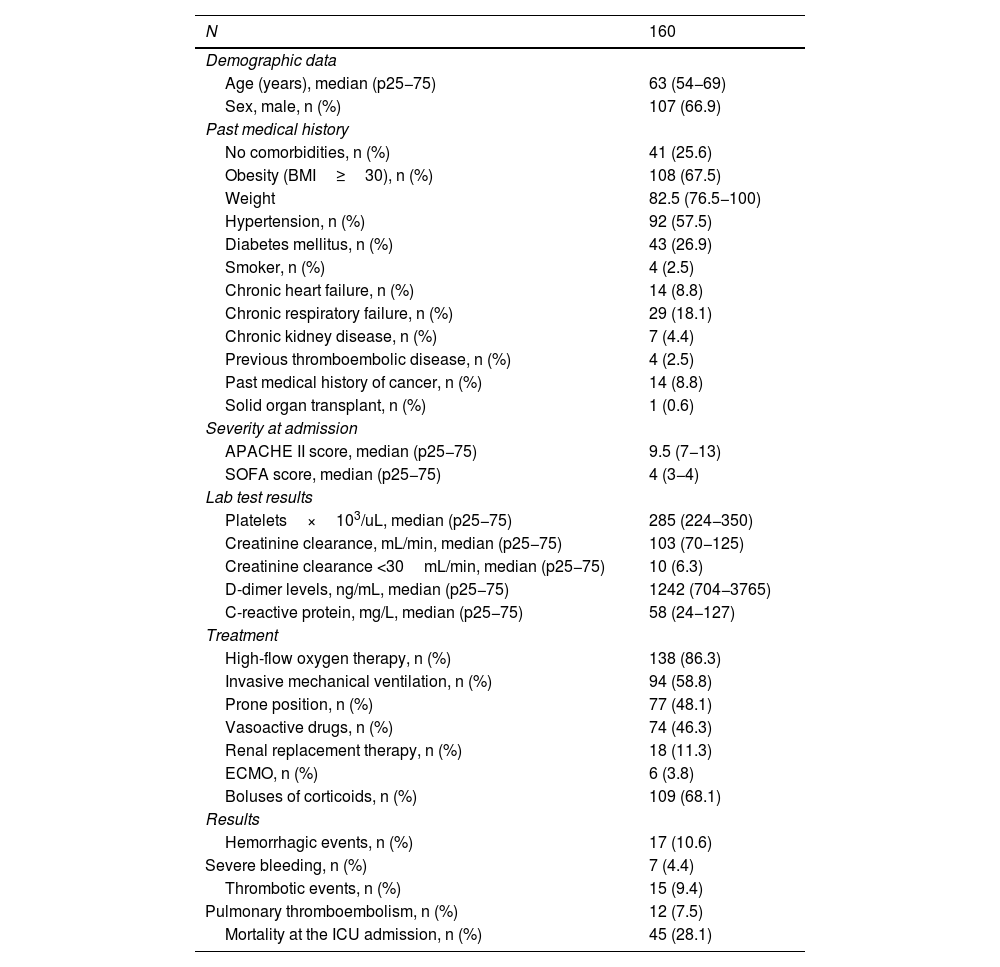
Clinical characteristics of the patients.
| N | 160 |
|---|---|
| Demographic data | |
| Age (years), median (p25−75) | 63 (54−69) |
| Sex, male, n (%) | 107 (66.9) |
| Past medical history | |
| No comorbidities, n (%) | 41 (25.6) |
| Obesity (BMI≥30), n (%) | 108 (67.5) |
| Weight | 82.5 (76.5−100) |
| Hypertension, n (%) | 92 (57.5) |
| Diabetes mellitus, n (%) | 43 (26.9) |
| Smoker, n (%) | 4 (2.5) |
| Chronic heart failure, n (%) | 14 (8.8) |
| Chronic respiratory failure, n (%) | 29 (18.1) |
| Chronic kidney disease, n (%) | 7 (4.4) |
| Previous thromboembolic disease, n (%) | 4 (2.5) |
| Past medical history of cancer, n (%) | 14 (8.8) |
| Solid organ transplant, n (%) | 1 (0.6) |
| Severity at admission | |
| APACHE II score, median (p25−75) | 9.5 (7−13) |
| SOFA score, median (p25−75) | 4 (3−4) |
| Lab test results | |
| Platelets×103/uL, median (p25−75) | 285 (224−350) |
| Creatinine clearance, mL/min, median (p25−75) | 103 (70−125) |
| Creatinine clearance <30mL/min, median (p25−75) | 10 (6.3) |
| D-dimer levels, ng/mL, median (p25−75) | 1242 (704−3765) |
| C-reactive protein, mg/L, median (p25−75) | 58 (24−127) |
| Treatment | |
| High-flow oxygen therapy, n (%) | 138 (86.3) |
| Invasive mechanical ventilation, n (%) | 94 (58.8) |
| Prone position, n (%) | 77 (48.1) |
| Vasoactive drugs, n (%) | 74 (46.3) |
| Renal replacement therapy, n (%) | 18 (11.3) |
| ECMO, n (%) | 6 (3.8) |
| Boluses of corticoids, n (%) | 109 (68.1) |
| Results | |
| Hemorrhagic events, n (%) | 17 (10.6) |
| Severe bleeding, n (%) | 7 (4.4) |
| Thrombotic events, n (%) | 15 (9.4) |
| Pulmonary thromboembolism, n (%) | 12 (7.5) |
| Mortality at the ICU admission, n (%) | 45 (28.1) |
APACHE, Acute Physiology and Chronic Health Evaluation; BMI, body mass index; COVID-19, coronavirus 2019; ECMO, extracorporeal membrane oxygenation; ICU, intensive care unit; SOFA, Sequential Organ Failure Assessment.
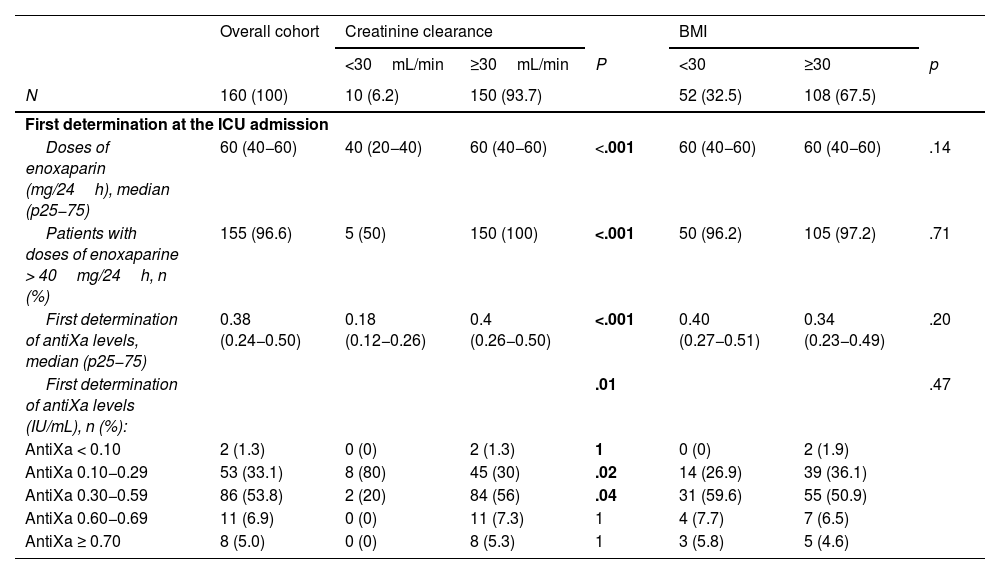
Table 2 shows the doses of enoxaparin received and the Anti-Xa factor values obtained at the first determination and at the ICU stay. When the first determination was performed, the median dose of enoxaparin administered was 60mg/24h (p25−75, 40−60). In relation to these doses, the first determination of Anti-Xa factor levels had a median of 0.28 IU/mL (0.34−0.50). A total of 53% of the patients (85/160) were within the target range of 0.30 IU/mL to 0.59 IU/mL.
Doses of prophylactic enoxaparin and AntiXa factor levels in critical patients.
| Overall cohort | Creatinine clearance | BMI | |||||
|---|---|---|---|---|---|---|---|
| <30mL/min | ≥30mL/min | P | <30 | ≥30 | p | ||
| N | 160 (100) | 10 (6.2) | 150 (93.7) | 52 (32.5) | 108 (67.5) | ||
| First determination at the ICU admission | |||||||
| Doses of enoxaparin (mg/24h), median (p25−75) | 60 (40−60) | 40 (20−40) | 60 (40−60) | <.001 | 60 (40−60) | 60 (40−60) | .14 |
| Patients with doses of enoxaparine > 40mg/24h, n (%) | 155 (96.6) | 5 (50) | 150 (100) | <.001 | 50 (96.2) | 105 (97.2) | .71 |
| First determination of antiXa levels, median (p25−75) | 0.38 (0.24−0.50) | 0.18 (0.12−0.26) | 0.4 (0.26−0.50) | <.001 | 0.40 (0.27−0.51) | 0.34 (0.23−0.49) | .20 |
| First determination of antiXa levels (IU/mL), n (%): | .01 | .47 | |||||
| AntiXa < 0.10 | 2 (1.3) | 0 (0) | 2 (1.3) | 1 | 0 (0) | 2 (1.9) | |
| AntiXa 0.10−0.29 | 53 (33.1) | 8 (80) | 45 (30) | .02 | 14 (26.9) | 39 (36.1) | |
| AntiXa 0.30−0.59 | 86 (53.8) | 2 (20) | 84 (56) | .04 | 31 (59.6) | 55 (50.9) | |
| AntiXa 0.60−0.69 | 11 (6.9) | 0 (0) | 11 (7.3) | 1 | 4 (7.7) | 7 (6.5) | |
| AntiXa ≥ 0.70 | 8 (5.0) | 0 (0) | 8 (5.3) | 1 | 3 (5.8) | 5 (4.6) | |
| N | 160 (100) | 22 (13.7) | 138 (86.2) | 52 (32.5) | 108 (67.5) | ||
|---|---|---|---|---|---|---|---|
| At the ICU admission | |||||||
| Mean dose of enoxaparin (mg/24h), median (p25−75) | 60 (53−73) | 60 (40−66) | 60 (53−73) | .10 | 60 (40−70) | 60 (55−80) | .01 |
| Mean levels of AntiXa, median (p25−75) | 0.48 (0.39−0.59) | 0.48 (0.35−0.57) | 0.48 (0.39−0.60) | .80 | 0.47 (0.39−0.57) | 0.49 (0.39−0.6) | .90 |
| Mean levels of AntiXa (IU/mL), n (%): | .48 | .93 | |||||
| AntiXa < 0.10 | 2 (1.3) | 1 (4.5) | 1 (0.7) | 1 (1.9) | 1 (0.9) | ||
| AntiXa 0.10−0.29 | 18 (11.3) | 3 (13.6) | 15 (10.9) | 6 (11.5) | 12 (11.1) | ||
| AntiXa 0.30−0.59 | 100 (62.5) | 13 (59.1) | 87 (63) | 33 (63.5) | 67 (62) | ||
| AntiXa 0.60−0.69 | 29 (18.1) | 3 (13.6) | 26 (18.8) | 7 (13.5) | 22 (20.4) | ||
| AntiXa ≥ 0.70 | 11 (6.9) | 2 (9.1) | 9 (6.5) | 5 (9.6) | 6 (5.6) | ||
| Number of determination of the AntiXa levels/patient, median (p25−75) | 3 (2−5) | 4 (3−9) | 3 (2−5) | .02 | 3 (1.5−4) | 2 (3−5.5) | .31 |
BMI, body mass index; COVID-19, coronavirus 2019.
During the rest of the stay, the dose of prophylactic enoxaparin was adjusted based on the Anti-Xa factor levels within the target range of 0.30 IU/mL to 0.59 IU/mL. The mean Anti-Xa factor level was 0.48 IU/mL (0.39−0.59). A total of 62% (100/160) of the patients fell within the target range (0.30 IU/mL to 0.59 IU/mL) while 25% (24/160) within ranges ≥0.60 IU/mL. Enoxaparin doses > 60mg/24h (OR, 4.57; 95%CI, 3.17–6.60; P < .001) and C-reactive protein levels < 175mg/dL (OR, 2.30; 95%CI, 1.28–4.11; P = .002) were independently associated with an increased risk of obtaining Anti-Xa factor values ≥0.60 IU/mL (above the target range) in the multivariate analysis (Supplementary Table S1).The median adjusted enoxaparin dose at the stay was 60 (53−73) mg/24h, which is significantly higher in patients with BMI>30 of 60 (55−80) mg/24h vs. 60 (40−70) mg/24h (P=.01). No variables independently associated with the development of thrombotic events were seen (Supplementary Table S2).
Currently, new studies on the management and prevention of thrombosis in patients with COVID-19 are being published like the INSPIRATION, REMAP-CUP, ATTACC, ACTIV-4a, etc. However, key aspects such as the appropriate dose of LMWH and possible optimization through Anti-Xa factor levels2,3 have not yet been clarified. In our experience, we saw that although steering the dose of prophylactic enoxaparin resulted in 62% of patients having mean Anti-Xa factor levels within the target range, 25% showed higher ranges (≥0.60 IU/mL). Higher doses of heparin (enoxaparin >60mg/24h) and lower C-reactive protein levels (<175mg/dL) were independently associated with a higher risk of overdose. Bösch J et al. found that elevated C-reactive protein values can play a role in resistance to LMWH activity, which could explain why patients from our study with lower values were more exposed to overdose.8 Although levels above the target range can potentially pose a greater risk of complications, only 6% had levels ≥0.70 IU/mL, and the rate of major bleeding was 4%, not particularly higher compared to that described in the medical literature (2%–6%).6,7,9
In this study, the dose of enoxaparin administered at the ICU stay was 60mg/24h (p25−57, 50−73mg). These doses are similar to those reported in former studies (median, 60mg/24h, 50mg/24h to 80mg/24h) that used monitoring with similar target levels (0.4 IU/mL to 0.5 IU/mL) 6. Mohamed A et al. found a high rate of overdose (48%) when intermediate doses (0.5mg/kg/12h) are administered—which is one of the strategies recommended in the medical literature available—and the Anti-Xa levels are monitored.3,7 The risk of overdose could have been higher if this regimen had been used without monitoring given the high rate of obesity (67%) and elevated levels of acute phase reactants found in our cohort.2,3,7
Finally, the objective of steering the dose of enoxaparin based on the Anti-Xa factor is to reduce the risk of thrombotic events. We should mention that, in our study, we found rates of 9%, which is the lower border limit of what has been reported by the medical literature available (9%–26%). However, this analysis is limited because we did not conduct a systematic search for thrombotic events meaning that some events may have been underdiagnosed.2,3
We are aware of the limitations of the study as it is observational and retrospective in nature and includes a non-systematic search for thrombotic events. Also, the size of its sample is limited. In addition, the target range proposed, although similar to that from former studies, is controversial with significant variability in publications (eg, surgical patients, 0.1 IU/mL to 0.3 IU/mL vs other COVID-19 studies, 0.3 IU/mL to 0.7 IU/mL).5,10 Still, we believe that this clinical experience can be useful regarding the design of future studies.
In conclusion, in this study of critically ill patients with COVID-19-induced pneumonia, the Anti-Xa factor levels obtained at the ICU stay allowed us to adjust doses of prophylactic enoxaparin. Nonetheless, there is a high risk of overdose especially in patients with higher enoxaparin doses and lower C-reactive protein levels.
Ethics of this scientific publicationThis study has been approved by Hospital Universitario Reina Sofía Ethics Committee (Code 010408). The need for informed consents was not deemed necessary given the observational and retrospective nature of the study.
FundingNone whatsoever.
Conflicts of interestNone reported.
the authors wish to thank Prof. Manuel Rodríguez Peralvarez and Dr. Rafael León López for their support in the statistical analysis of data.