Plato used to say: «look for, and you will find», and this is applicable to the diagnosis of pulmonary aspergillosis at the intensive care unit (ICU) setting. It is risky to make any wise statements on its incidence rate without having to ask first on the diagnostic methods applied. On the one hand, if we don’t conduct an active search, we run the risk of underdiagnosing the disease. On the other hand, if we’re talking about a targeted search, we could be making a mistake by diagnosing colonizations as infections.
Most studies on the incidence rate of aspergillosis have been conducted by analyzing retrospective databases whose primary endpoint was not looking for this etiology. Although some authors report on a low incidence rate of aspergillosis in the critically ill patient,1,2 this conclusion can be erroneous if we assume that these studies are only based on isolating a species of Aspergillus in a respiratory sample. In a recent European multicenter study conducted among intubated patients with pneumonia due to Influenza, a higher incidence rate compared to the one found in the analysis conducted by Claveria et al.3 has been reported. This maybe explained partially because they analyzed patients on mechanical ventilation for over 48 h,4 and not within the first 24 h after ICU admission.
On the other side of the spectrum, we find studies that have conducted an active search for aspergillosis where the incidence rate documented can be up to 20 times higher.5 In these studies the microbiological diagnosis was not exclusively limited to the isolation of fungus in the culture adding the determination of biomarkers like galactomannan to the bronchoalveolar lavage sample and serum.
The diagnosis of pulmonary aspergillosis in the critically ill patient is an unsolved challenge for clinicians. In the first place, because the clinical and radiological criteria can remedy other etiologies. It is essential to have previous suspicion of the disease and lean on a targeted microbiological diagnostic strategy.
There is no doubt that reducing the criteria of fugal isolation in the respiratory sample leads to the risk of underdiagnosing aspergillosis. These criteria are considered the reference microbiological diagnostic method and they are the entry criterion contemplated in the AspICU criteria proposed by Blot et al.6 These criteria were proposed to better identify critically ill patients compared to those recommended by the European Organization for Research and Treatment of Cancer/Mycosis Study Group (EORTC/MSG).7 However, we know that fungal growth in cultures is slow and can delay the beginning of treatment until testing positive. Cultures have low sensitivity (<65%), can be altered by contaminations, and produce false negatives if the patient is on antifungal treatment. The main advantage of cultures would be to allow the performance of an antifungogram to know the in vitro sensitivity to antifungal drugs.
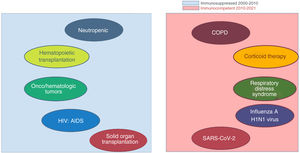
Also, we should mention how important the quality of the respiratory sample really is in the aforementioned studies that show such a low incidence rate of aspergillosis. The tracheal aspirate was the most widely used respiratory sample of all. There is no doubt that this is a key factor since it contributes to a low-quality search strategy. Drawing non-invasive respiratory samples is limited by the fact that it does not include damage to the pulmonary parenchyma. To this date, the bronchoscopic bronchoalveolar lavage is the top-quality sample after pulmonary biopsy whose indication in critically ill patients is often anecdotal. Diagnostic fiber bronchoscopy in patients on mechanical ventilation is a safe technique with very few complications when performed by experienced personnel.8 In their study, Claverias et al.3 conclude that in risk patients an active strategy to search for pulmonary aspergillosis should be implemented. Fig. 1 shows the clinical profile of patients admitted to the ICU that could be considered as risk patients. In nearly a decade, different profiles of patients compared to the traditional profile have appeared represented by neutropenic and/or immunosuppressed patients. We should mention that this condition is not exclusive to show pulmonary aspergillosis. Therefore, suspicion should be independent from the immune status of the critically ill patient.
Therefore, we should take into consideration these new profiles of patients without immunosuppression and think that in the absence of neutropenia, the clinical and radiographic expression of the disease vary same as microbiological diagnostic methods like the determination of serum galactomannan that is less useful.9
If we are looking into what the optimal approach should be, and we decide to move on with an active search for aspergillosis at the ICU setting the following is advised: we should be taking into consideration the risk profiles confirmed and draw a new respiratory sample with diagnostic yield that in decreasing order of quality would be: bronchoscopic bronchoalveolar lavage (that allows taking a targeted sample from the lower respiratory tract), and bronchoalveolar mini-lavage (whose greatest advantage is that no experienced personnel is required). However, its setback is that is a non-targeted blind technique. On the other hand, the diagnostic sensitivity of tracheal aspirate has proven inferior in the upper airway. Finally, we should not be limited to microbiological culture as it is necessary to expand the study by adding the determination of biomarkers like the determination of galactomannan in bronchoalveolar lavage in the respiratory sample drawn.10
By widening these search criteria and using all the resources available at each center such as fresh specimen staining, culture, biomarkers determination, lateral flow assay, and CRP determination we can begin treatment early.11
The clinical situation should determine whether antifungal treatment should be started or not. However, in critically ill patients who need invasive ventilation and with gas exchange disorders and hypoxemia we should think of fighting the high mortality rate reported to this date. The positive results obtained in some of the microbiological tests recommended in a patient without hypoxemia with favorable clinical progression and in the process of weaning from the ventilator should make us think that we’re dealing with a colonization and, therefore, avoid administering antifungal drugs.
It would be interesting to know whether by implementing these strategies for the active search of pulmonary aspergillosis at the ICU setting the incidence rate of this serious infectious complication changes. The variability seen in the incidence rate reported in the medical literature available makes us assume that research includes methodological errors that should pave the way towards knowledge. To know the actual incidence rate descriptive, longitudinal, and prospective follow-up studies should be designed including the entire diagnostic arsenal available to us.
FundingNone whatsoever.
Please cite this article as: Estella Á. Aspergilosis pulmonar en la unidad de cuidados intensivos: ¿una enfermedad infradiagnosticada? Med Intensiva. 2022;46:423–425.