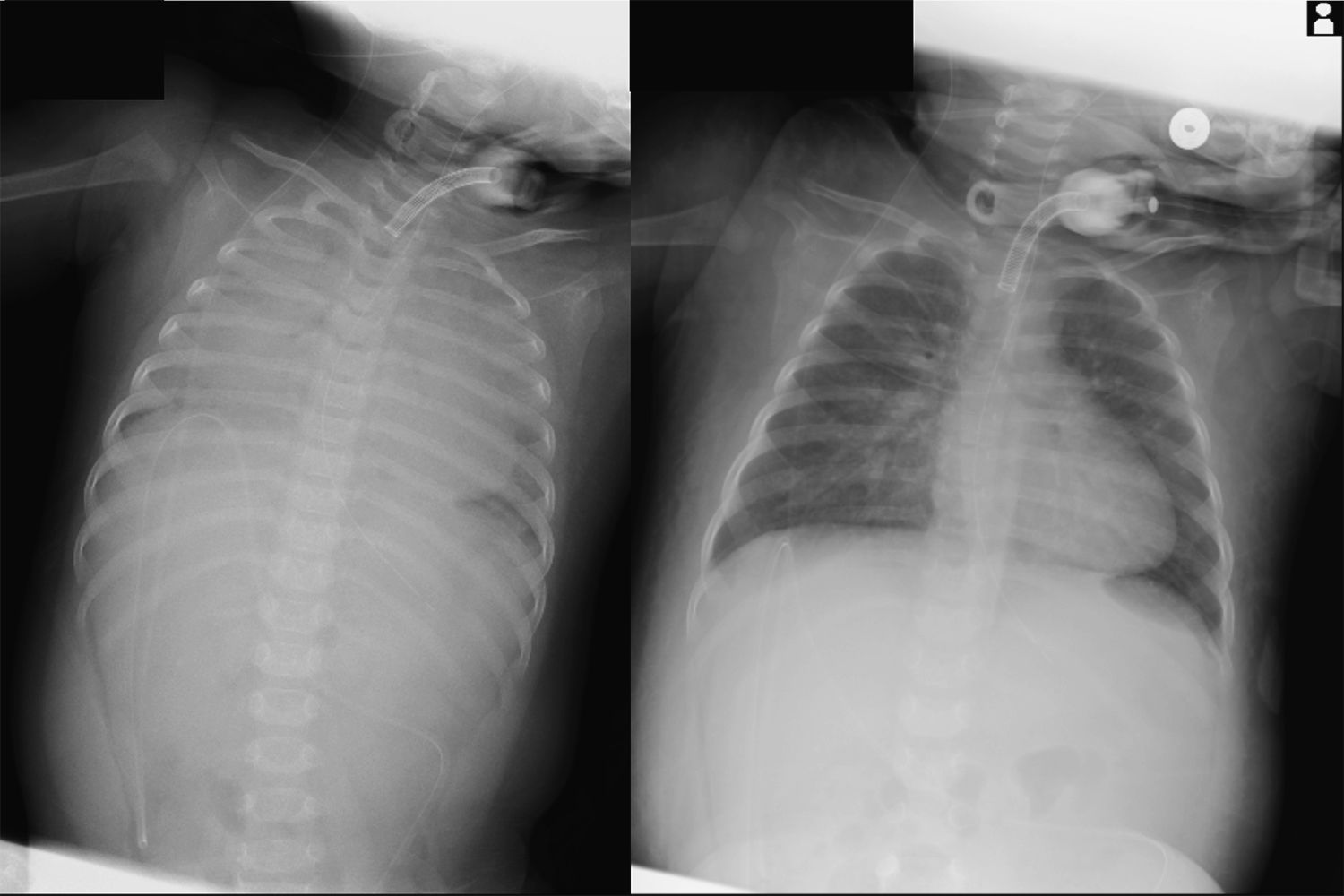
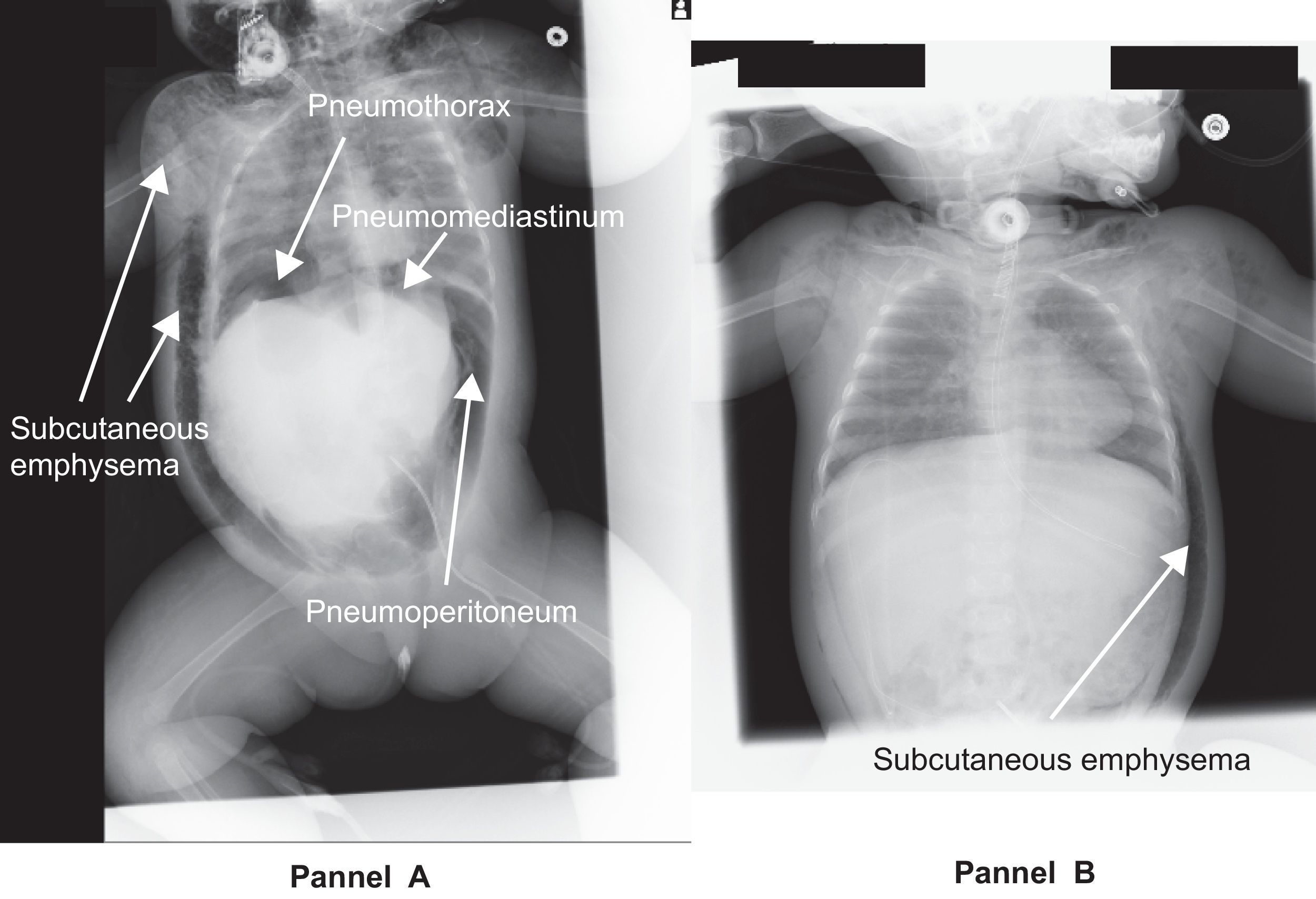
An 8-month-old female maintained on conventional mechanical ventilation via a tracheostomy while at home was admitted to the intensive care unit of our hospital due to acute respiratory distress syndrome (ARDS). The uncuffed tracheostomy tube was replaced with a cuffed tube and airway pressure release ventilation (APRV) was initiated Her respiratory status gradually improved over the following 2 days (Fig. 1). On the 4th day of hospitalization, the patient experienced acute respiratory deterioration; this was ultimately attributed to patient-ventilator asynchrony. APRV with higher PEEP was reinstated. On the same day, we observed sporadic hemodynamic instability and the patient developed a tense and distended abdomen. A chest-abdominal radiograph revealed free air under the diaphragm and subcutaneous emphysema with pneumothorax and pneumomediastinum (Fig. 2A). APRV was discontinued immediately and the patient was switched over to conventional PCV. The patient withstood this temporary derangement, and systemic pneumatosis resolved gradually with conservative treatment. She was ultimately weaned from mechanical ventilation at the hospital and returned to routine mechanical ventilation at home although subcutaneous emphysema persisted (Fig. 2B). In conclusion, although there are certainly benefits provided by APRV, severe lung injury may develop in pediatric patients, most notably in association with patient-ventilator asynchrony.
Authors’ contributionsAll authors were involved in the treatment of the patient. TI and SI collected patient data, drafted the manuscript, and obtained the consent for publication from the patient's next of kin. MK revised and edited the manuscript. All authors contributed and approved the final version.
FundingThis study was supported only by departmental funding from our institution.
Conflict of interestsThe authors declare having no competing interests.